Rural Mortality Rates: A Cause for Concern

by: Julia Stullken, Master of Public Health student
A recent report in the American Journal of Public Health discusses the importance of where a person lives in determining health. Researchers describe a growing “rural mortality penalty,” characterized by a shift in mortality rate disparities from urban to rural populations. That is to say, over the past 50 years as urban health initiatives have been improving, rural health has not been able to keep up. Even after adjusting for factors like race, age, and education level, mortality rates were still significantly higher in rural areas. Furthermore, the study concluded that when rural locales are combined with high-percentage poverty, mortality rates are even higher, and climbing.
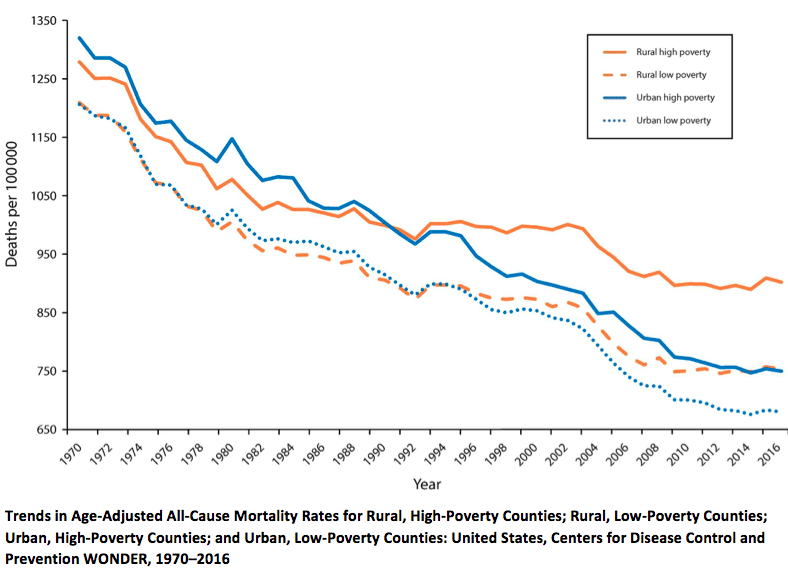
Don’t be fooled by the negative slope in this figure. What is striking about the graph is that deaths in rural high-poverty populations are declining at a much slower rate than deaths in urban populations. This is likely because access to health care and the ability to afford that care are much lower in rural high-poverty populations; many of these individuals still don’t have healthcare. Another possibility could be the increasing deaths related to opioid addiction, which are higher in rural areas.
So What?
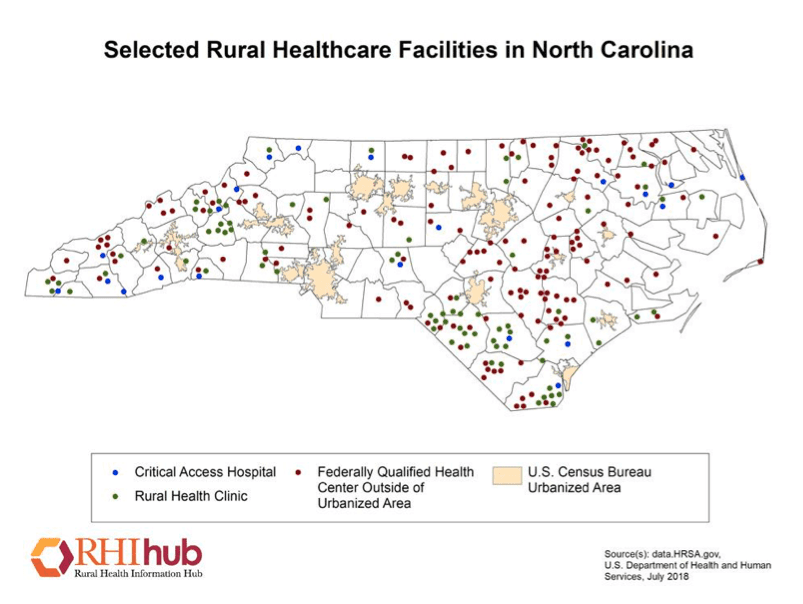
This research is important for North Carolina, considering most of the state is rural. According to the USDA Economic Research Survey, almost 19% of rural North Carolinians are living in poverty (about 5% more than their urban counterparts). As illustrated in the map from the Rural Health Information Hub, many of the rural counties in North Carolina have few or no healthcare facilities.
What does all this mean for Charlotte and other urban centers? Since poverty and education are undeniably linked, support and collaboration between urban and rural organizations should be maximized to provide literacy and education resources to rural communities. Institutions like UNC Charlotte should encourage students pursuing careers in public health, health administration, education and nursing, among other fields, to consider working with rural populations after graduation. Additionally, large healthcare facilities should maximize use of telemedicine and mobile screening units to provide care to rural populations.
Sources:
American Journal of Public Health
Graph: Cosby, A., McDoom-Echebiri, M., James, W., Khandekar, H., Brown, W., Hanna, H., (2019). “Growth and Persistence of Place-Based Mortality in the United States: The Rural Mortality Penalty”, American Journal of Public Health. 109(1), 155-162. DOI: 10.2105/AJPH.2018.304787
USDA Economic Research Service